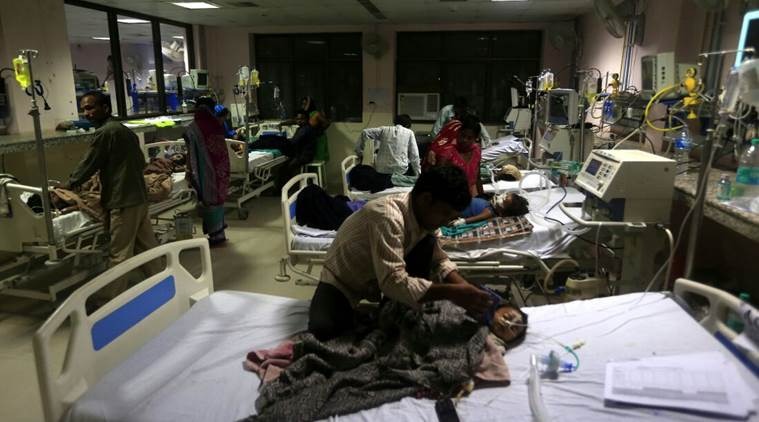
Nearly four years after the Covid‑19 pandemic exposed deep structural weaknesses in the country’s public health system
As the Union Budget for the upcoming fiscal year approaches, healthcare once again finds itself at a critical juncture in India’s policy discourse. Nearly four years after the Covid‑19 pandemic exposed deep structural weaknesses in the country’s public health system, expectations from Budget 2026 are high but tempered by the reality of slow, incremental reform. While successive budgets have acknowledged health as a national priority, data suggests that fiscal commitment has not yet matched the scale of India’s healthcare challenges, particularly for rural populations, informal workers, women, and other marginalised communities.
India’s public health expenditure has remained stubbornly low. In recent years, government spending on health has hovered around 1.1 to 1.2 pc of GDP, far below the 2.5 pc target committed under the National Health Policy and much below the 8-10 pc invested by developed economies and less than a third of even the levels recommended by the World Health Organisation.
However, in India, the investment in real terms has only declined in the past decade or so. In absolute terms, the Union health budget has seen nominal increases year after year, but these rises have largely been offset by population growth, rising disease burden, and medical inflation, which industry estimates place at roughly 12 pc annually. As a result, India continues to rely heavily on out‑of‑pocket expenditure, which accounts for close to 50 pc of total health spending, pushing millions of households into financial distress each year.
Also Read: Union Budget 2025: Stakeholders push for increased healthcare funding
Looking back at last year’s Union Budget, Sandeep Chachra, Executive Director of ActionAid Association, says the allocations reflected continuity rather than transformation. “The Budget showed the much‑needed and continued concern for healthcare as a national priority in the post-pandemic period. However, in face of the need, the increase was more incremental in nature, with both the scale and structure of allocations falling short of what is required to address India’s deep‑rooted health inequities,” Chachra tells Media India Group.

Sandeep Chachra
According to Chachra, while headline numbers rose, the underlying fiscal prioritisation did not significantly shift, leaving public health expenditure stalled well below stated policy goals.
Some tangible progress has nevertheless been visible on the ground, especially in areas shaped by the urgency of the pandemic. Investments in oxygen infrastructure, emergency preparedness, and digital health platforms expanded rapidly between 2020 and 2023. Civil society organisations played a complementary role. According to Chachra, ActionAid Association supported the strengthening of public hospitals by installing oxygen generation plants and distributing oxygen concentrators across 164 districts in 13 states during the Covid-19 crisis. These interventions, Chachra says, demonstrated how targetted public investment can deliver immediate, life‑saving outcomes when aligned with community needs.
Yet, much of this expansion has been crisis‑driven rather than systemic. Core public health functions primary healthcare, preventive services, nutrition, and mental health remain chronically underfunded.
Rural India continues to face shortages of functional Primary Health Centres and Community Health Centres, while district hospitals struggle with inadequate staffing and equipment. Data from government sources has consistently pointed to gaps in human resources, with significant shortfalls of doctors, nurses, specialists, and mental health professionals across states.
Compounding these challenges is the fiscal strain on states. Over the past decade, transfer of funds from the Union government to states for health have declined as a share of overall spending, falling to a decadal low of around 43 pc in 2024-25. This has weakened state capacity to sustain and expand services, even though states bear the primary responsibility for healthcare delivery. “The erosion of fiscal support has directly affected the ability of states to maintain essential services,” says Chachra, adding that any meaningful reform must include stronger fiscal decentralisation.
Also Read: India’s budget for mental health leaves a lot to be desired
The coming budget is therefore being viewed as an opportunity to move from incrementalism to structural reform. For Chachra, a central expectation is a clear, time‑bound commitment to raise public health expenditure to at least 2.5 pc of GDP. Such an increase, Chachra says, is essential to address India’s demographic realities, disease burden, and persistently high medical inflation. Without this shift, inequalities will continue to deepen, forcing vulnerable households to absorb rising out‑of‑pocket costs and exposing them to catastrophic health expenditure.
For marginalised communities, the consequences of underinvestment are severe. Illness often translates into lost income, indebtedness, and long‑term insecurity, particularly for informal workers and women. Climate‑related stresses are intensifying these risks, with heat stress, vector‑borne diseases, and malnutrition adding new pressures to an already overstretched system. Despite these trends, public health planning has been slow to integrate climate resilience into routine healthcare delivery.
Technology, many experts says, could play a transformative role if backed by regulation and funding. Sujeet Katiyar, Director of Surisolis Ventures, believes digital health is key to bridging India’s rural‑urban divide, where nearly 70 pc of the population lives in rural areas but close to 80 pc of advanced healthcare infrastructure is concentrated in cities.

Sujeet Katiyar
“Nearly 70 pc of India’s population lives in rural areas, while close to 80 pc of quality healthcare infrastructure is concentrated in urban centres. This gap simply cannot be bridged without the use of technology be it telemedicine, digital diagnostics, electronic health records, or AI-driven clinical tools. However, the moment technology enters healthcare, issues of data privacy, cybersecurity, patient safety, and algorithmic accountability become central,” Katiyar tells Media India Group.
However, Katiyar is blunt about the gaps in regulatory oversight.
“The current allocation does not sufficiently address patient safety, data privacy, cybersecurity, or quality assurance. These are severely underfunded areas,” he says.
While India has initiated steps such as the Digital Personal Data Protection framework and discussions around AI regulation, enforcement capacity remains limited. In the absence of robust governance, overseas players are able to offer subsidised digital health services primarily to collect data, raising concerns about sovereignty, privacy, and patient safety.
India generates an estimated 20 pc of the world’s digital data but hosts only about 2 pc of global data‑storage infrastructure. This imbalance, experts warn, makes the health system particularly vulnerable to data breaches and cybercrime. High‑profile ransomware attacks on healthcare institutions in recent years have exposed the lack of breach preparedness and response mechanisms. Katiyar stresses the need for budgetary allocations specifically earmarked for digital compliance, cybersecurity infrastructure, and algorithmic accountability.
Also Read: Healthcare, education again ignored in Union Budget
Accountability, he adds, remains a grey area in AI adoption. If an AI tool deployed in a hospital leads to an adverse outcome, responsibility is often unclear, deterring hospitals from adopting technology at scale.
“Before AI reaches patients, there must be evaluation, clinical validation, and certification by a competent authority,” Katiyar says, pointing to regulatory models in the United States and Europe. Incentives for compliant adoption, he suggests, could accelerate responsible use while improving outcomes.
Legal experts echo these concerns. Biplab Lenin, Partner (Pharma, Healthcare and Life Sciences) Cyril Amarchand Mangaldasa, notes that while last year’s budget maintained healthcare spending at around 2 pc of GDP and continued flagship programmes such as Ayushman Bharat, outcomes in Tier‑II and Tier‑III cities have been uneven. Capacity constraints at state and municipal levels, along with manpower shortages, continue to limit last‑mile delivery.

Biplab Lenin
Experts attribute this unevenness to state and municipal capacity constraints, as well as persistent shortages in healthcare manpower. India has approximately one government doctor for every 11,000 people, far below the World Health Organisation’s recommended ratio of one doctor per 1,000. Nursing shortages are equally acute, while gaps in diagnostic equipment and operational funding continue to limit the effectiveness of public facilities. As a result, even where infrastructure exists, last-mile service delivery remains weak.
Against this backdrop, expectations from the upcoming Union Budget are centred on strengthening the foundations of public healthcare rather than announcing new headline schemes. Legal and policy experts argue that targetted investment in primary healthcare particularly in rural and developing districts must become the core focus.
Also Read: World Health Day: Sedentary lifestyle, stress, stigma leads to rising cases of PCOS in India
“The key expectation from the upcoming budget is targetted strengthening of primary healthcare, particularly in rural and developing districts. Digital health tools such as electronic health records and telemedicine can support access, but only if they are accompanied by sustained investments in connectivity, training and frontline integration,” Lenin tells Media India Group.
Without operational funding and skilled personnel, infrastructure expansion alone cannot translate into improved health outcomes, he adds.
Maternal and child health remains another area where gaps persist. While multiple schemes exist, fragmentation, weak referral systems, and inconsistent quality of care continue to undermine effectiveness. Mental health, in particular, remains a blind spot, with limited community‑based services and poor integration into primary care. Despite growing evidence that primary healthcare is the most cost‑effective route to reducing morbidity and mortality, it has yet to receive commensurate fiscal prioritisation.
There is broad consensus among experts that the focus must shift from launching new schemes to executing existing ones effectively. Predictable funding for primary care, improved centre‑state coordination, and deeper integration of digital health into routine public services are emerging as key demands. Equally important is investment in frontline health workers, such as ASHAs, Anganwadi workers, and ANMs through regularised employment, fair wages, and social security.
Gaps in primary care are also reflected in maternal, child, and mental health outcomes. While institutional deliveries now account for over 85 pc of births nationwide, maternal mortality remains elevated in several states, and child malnutrition continues to pose a major public health challenge. Data from national surveys indicates that more than one-third of Indian children under five are stunted, while anaemia affects a majority of women of reproductive age. Nutrition-related disorders contribute significantly to the country’s overall disease burden, yet public spending remains skewed toward curative care rather than integrated nutrition and prevention.
“The data makes it clear that India is paying a high price for neglecting primary and preventive healthcare. When PHCs lack staff, diagnostics, and medicines, people are pushed into private care for conditions that should be treated early and close to home. This is why out-of-pocket spending remains so high and why health shocks so often translate into long-term poverty. Strengthening primary care, nutrition, and community-based mental health services is not just a social imperative it is the most economically rational investment the health system can make,” says Chachra.
