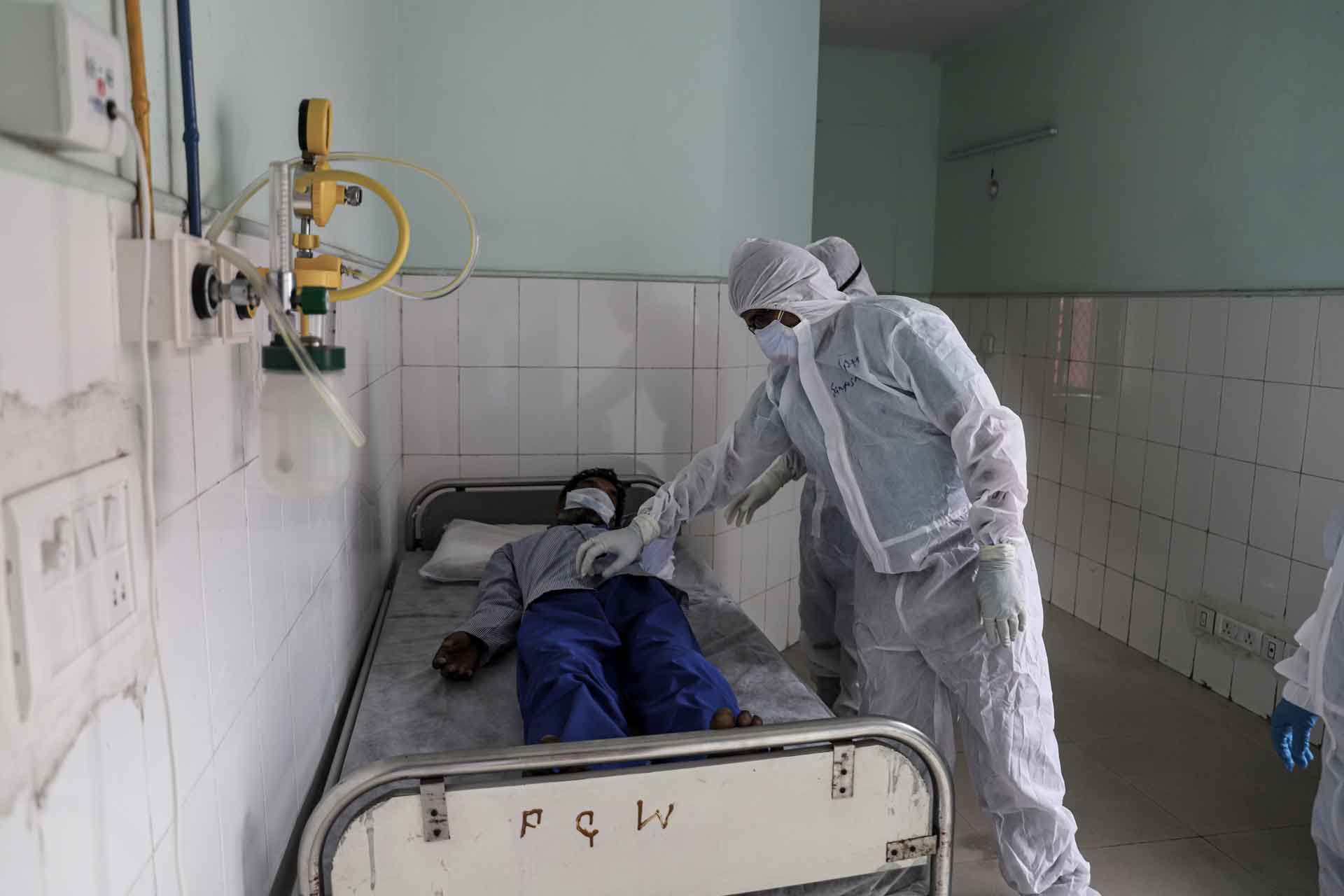
Access to hospitals and healthcare may be rare in India, but it still leads in AMR deaths (MIG Photo)
An alarming report published earlier this year in The Lancet, a medical journal, said that antimicrobial resistance was directly responsible for 1.27 million death and linked to about 4.95 million other deaths across the world in 2019. Antimicrobial resistance is when bacteria causing serious diseases, for instance tuberculosis, become resistant to the drugs used to treat the illness. The bacteria become resistant if a particular drug is overused in a particular community, which often makes the doctors prescribe even more powerful combinations of medicines and eventually all of them prove to be ineffectual. Most of the deaths were caused by drug resistance in lower respiratory infections such as pneumonia, followed by bloodstream infections and intra-abdominal infections.
Conventional wisdom would have it that rich countries, with their modern drugs, wide availability as well as financial capacity would be the largest victims of this resistance. However, surprisingly antimicrobial resistance cases were found the most in two of the poorest parts of the world – sub-Saharan Africa and South Asia. One in five deaths in these regions is in children below five years of age.
This is partly due to the fact in these two regions, relatively low-priced generic drugs are easily and widely available, without any prescription and without any supervision. This misuse combined with lack of clean water and sanitation as well as prevention and control of infections leads to spread of microbes, some of which are resistant to the antimicrobial treatment.
The spread of AMR, as the phenomenon is called, is so rapid that experts now believe that they had severely underestimated the dangers posed by it. Initial predictions were of AMR causing 10 million deaths by 2050. But now scientists believe that this tragic milestone would be reached much faster, perhaps even in this decade. No wonder, then that the WHO has declared AMR as one of the 10 most significant threat to public health in the world and the wild-fire spread of AMRs witnessed so far would seriously undermine the UN Sustainable Development Goal of development and health for all by 2030.
Poor regulation, drug manufacturers and doctors
The blame for the widespread misuse of the antibiotics can be laid mainly at three doorsteps – of the government and regulatory bodies, the doctors and the drug manufacturers. The governments, especially in the developing world, have been lax to the point of criminal in poor regulation of the drug markets. In most of these countries, even the most powerful drugs, normally to be prescribed with caution by even the most experienced doctors in extremely rare situations, are freely available over the counter at the next-door drug store without any prescriptions needed.
Over the decades, as populations and the economies have grown, the number of pharmacies or drug stores has multiplied and with it the availability of drugs. The growth of drug manufacturing industries in some of the developing countries, notably India, which has emerged as the hub of low-priced and high-quality generic medicines.
With the generics being a fraction of the branded drugs with almost the same impact, the sale of generic medicines has boomed not just in the poor countries, but increasingly even the rich nations are turning to them to keep their spiralling healthcare costs under control.
To push their drugs, pharmaceutical companies have for long used dubious practices, developing extremely close relationships with doctors, ‘rewarding’ them for prescribing their drugs to the point that the rewards are nothing short of bribery, with overseas fully-paid vacations thinly veiled as ‘conference’ trips, fancy gadgets and everything short of cash for prescriptions.
As powerful antibiotics are more expensive than the others, doctors are often ‘incentivised’ to turn to them even where not needed or at least prolong the prescription period to far more than what may be needed.
But it is not just doctors, some patients, especially the wealthier ones, prefer that their doctors prescribe them the most powerful drug in the market, almost the ‘magic pill’, irrespective of the costs involved. Though the doctors can say they did not want to, but are only doing so to oblige their long-term patients, but by doing so they violate their Hippocratic oath of taking care of the patient and it is the doctor not the patient who ought to know what drug goes best for what kind of treatment.
Pandemic effect on AMR deaths
If the situation of AMR deaths was already alarming in 2019, before the onset of the Covid-19 pandemic, then it may have become even more serious, even critical over the past two years, due to two key factors.
One, the global healthcare sector and governments have been overwhelmed by the coronavirus, forcing them to ignore the other, pre-existing and equally mortal health-related challenges, leading healthcare activists to raise alarms about rise in deaths due to diseases like tuberculosis, measles or malaria as well as poor vaccination of infants against diseases like tetanus or polio.
The other and equally critical effect of Covid-19 has been that over the past two years, doctors the world over have turned to extremely powerful drugs, notably corticosteroids, like dexamethasone, hydrocortisone or prednisone, for severe infections, to tackle the unknown virus, especially in the way it rapidly spread between organs and led to deaths in matter of days.
More out of desperate attempts to save lives than anything else, millions of doctors around the world are believed to used or prescribed these medicines. However, corticosteroids, which are used in other severe illnesses, mainly to tackle inflammations of blood vessels and muscles, are already known to have serious side effects in most patients.
Their side effects are worse, even life threatening, when patients already have other ailments like diabetes, which is especially prevalent in the developing countries, notably India and the Middle East. Medical experts have cautioned against use of steroids for patients with diabetes or borderline diabetes, as it could lead to other infections, notably bacterial and fungal ones, creating more problems for the patients rather than solving them.
Unfortunately, during the various peaks of the pandemic, these steroids were in huge demand, leading to a thriving black market as drug manufacturing companies could not raise their production to meet the exponential growth in demand. More often than not, though these are meant to be delivered to patients by trained doctors and hence mainly used in hospitals or clinics, most of the sales were recorded in the street side stores and often with no prescriptions or even the prescription being used by dozens of people, desperate to get hold of anything that could save their loved ones. The prices of these steroids, at least in India during the deadly second wave in March-July 2021 shot up by 100 times the maximum retail price authorised by the government.
